An interview with a COVID-19 frontline nurse in New York
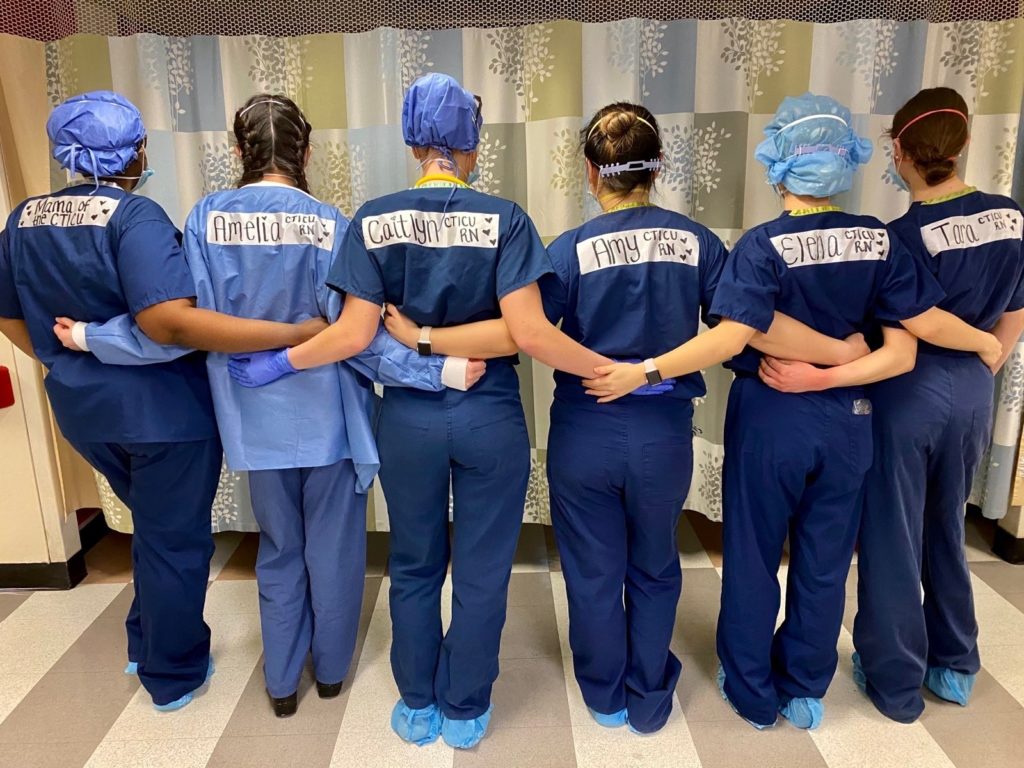
Amelia Conner qualified as a nurse two years ago at the University of Virginia. Her first job after graduating was in the cardio thoracic intensive care unit (ICU) at North Shore University Hospital, Manhasset, Long Island, New York
In her normal day job, Ms Conner looks after patients who are in hospital for cardiac surgery, mainly open-heart surgery.
Now, with two years of nursing experience, albeit in intensive care, she finds herself working at the sharp end, caring for people with COVID-19.
Most of the patients in her ward and the hospital’s other intensive care areas were quickly discharged and the hospital geared up for the expected sudden influx of extremely sick COVID-19 patients.
All of the hospital’s ICUs are now COVID-19 units, and all of its ICU nurses are now working with COVID-19 patients.
She says it’s hard to believe that the remarkable changes that have taken place have all happened in the past five or six weeks.
“Once the first ICU was converted, we knew what was coming. Our educators were coming around reminding us of our donning and doffing procedures for the personal protective equipment, and this training was backed up with some mandatory online education modules and some COVID-19 training.
‘I was the first nurse from my unit to be sent over to a COVID ward. My unit deals with ECMO [extracorporeal membrane oxygenation] patients, so as the first COVID ECMO patient arrived a colleague and I had to go. Our educators went up with us – it was on the day I finished the online modules!”
Patients on ECMO are at the most extreme end of the spectrum of care and are only given the treatment, which involves pumping and oxygenating the blood outside of the body, allowing the lungs to rest, when there are no other options for care.
“On my first day I was very nervous. The staff were all very nice to me – they called me ahead of my shift so that it wasn’t a surprise when I showed up for work. My educator and my manager came up with me to make sure that I was okay. It was a new unit for me, so they showed me where everything was and went over procedures. It was very helpful that I went with another nurse from my unit – It’s always nice to have someone you are comfortable with when you are going into a new situation.
‘I’ve been working in an ICU for two years, so I am used to that sort of environment, but it was definitely a new experience. It took some time getting used to. I’m familiar with treating ECMO patients, but I had to adjust to the environment and there were some new medications to get used to.
‘The COVID patients I usually look after are not on ECMO – that was the extreme, but almost all the patients I look after are on CPAP or ventilators. We look after the sickest patients – the patients on other units are not usually ventilated. Our patients are either on ventilators, have just come off ventilators or we suspect will shortly need ventilators.”
Ms Conner says working in such an environment in heavy, hot and uncomfortable PPE makes every day very demanding.
“The worst aspects of it all are the emotional and physical strain. Obviously, we are dealing with a lot of sick people, which we are used to, but it’s just on a much bigger scale. One of the hardest things is that, obviously for safety reasons, family members aren’t coming to visit. So now, the healthcare providers are the go-betweens between the patient and their families. That is an added stress for us: we are consoling family members and we are their only source of information, which is stressful for them and for us.
‘And coming in to do a shift on a COVID ICU is just so tiring. I usually do three 12-hour shifts, 7.00pm till 7.00am, but we come in earlier and leave later because we have to change before we go in and change again when we go home, so that adds an extra half-hour or hour to our regular shift.
‘I’m lucky that I live with my family and they are relatively healthy, but I know that some of my co-workers have family members who are compromised, so they can’t go home. That’s a really stressful thing for a lot of people who have to either stay somewhere else, or if they are at home, have to be quarantined from their family.
‘A few of my colleagues have got sick, but not as many people as I would have thought. We are lucky that those who got sick were not on the extreme end of the spectrum of COVID-19, and most of them have already recovered – they were out for a week or two with minor symptoms, so we are very lucky in that respect.”
Despite the pressures of the work and the emotional toll, Ms Conner says there are some positive things that have come out of the whole experience.
“I’m lucky because I had some experience of working with such sick patients before, and my co-workers are the best people – if it wasn’t for them, this would be so much harder. They are very supportive, and most of the time if we are working on an unfamiliar unit you usually go with somebody else, and at least have the support of somebody you know.
‘I have to say the support from my community has been great: I come from a small town, and people I don’t even know are reaching out to me, they are offering to buy food, sending us letters, you know, things that make us feel a little better. And our local fire department and the police officers mounted a fire guard for us, hanging flags off the ladders, which was really nice: my boyfriend is a firefighter, so he was there too. The support from the community has been really helpful.
‘And the husband of one of my co-workers, who is a therapist, has offered his services to nurses and other providers to reach out for counselling if we need it, which is nice.
‘Nurses are used to a certain amount of emotional strain, but this is definitely on a bigger scale. One of my best friends is a nurse in the unit and she made a positivity video which is really great. It has some uplifting music, some pictures of us all, and we are all there for each other.
‘We have a work group-chat where everyone sends reassuring things, whenever a patient leaves the unit, we share that. When someone gets discharged there’s a special chime that goes over the public address system so that everyone knows a patient is going home.
‘And when someone gets extubated and comes off the ventilator the hospital plays Here Comes the Sun by the Beatles. We discharged our thousandth patient last week, so they played Don’t Stop Believing by Journey over the PA, which was really fun, and that video went viral!
‘We have all matured in our nursing careers over the past few weeks’ experience and we have all learned a lot. I have dealt with things I would never have dealt with in my regular unit. One example is nursing patients in the prone position: since I work in open heart surgery, we would never prone a patient. Now that is something we have got used to and we do it all the time. It’s definitely been an experience for everybody, and one good thing that will come out of this is that we will all be better care providers. I’ve had the opportunity to work with people I probably wouldn’t have ever interacted with before, and it’s been nice to form new relationships with other teams. We will definitely take the skills we have learned through this time with us: wherever we go after this, we’ve all learned a lot.”
Where Ms Conner works, the pandemic seems to be on the retreat, but she is aware that nurses in other places may just be about to experience something similar to what she has been through. She has a simple message based on her experiences.
“Your patients are your first priority and you will want to do everything you can to help them, but it is important to handle things cautiously, to be safe and take your time to put on your PPE. Of course you want to protect your patients, but you also have to protect yourself.
‘So be safe, be smart, take your time to think things through and learn from your co-workers, because everyone has something to bring to the table – work as a team, and it will be okay. Take what you learn from one patient to the next and try to keep up to date with information that’s coming out all of the time.
‘And if you need help, ask for it: a lot of this is emotionally draining for everybody, and whatever you’re feeling, I’m sure someone else is feeling that way too. We are making our way through, and so long as you have the support of your co-workers, you will too.”

